This content is courtesy of Mayo Clinic, the No. 1 hospital in the nation according to U.S. News & World Report. Minnesota Oncology is a member of the Mayo Clinic Care Network. This relationship provides us with access to information, knowledge and expertise from Mayo Clinic.
Learn about moles (nevi), what causes them, whether they put you at increased risk of skin cancer and how to check a mole for signs of skin cancer.
Moles are a common type of skin growth. They often appear as small, dark brown spots and are caused by clusters of pigmented cells. Moles generally appear during childhood and adolescence. Most people have 10 to 40 moles, some of which may change in appearance or fade away over time.
Most moles are harmless. Rarely, they become cancerous. Monitoring moles and other pigmented patches is an important step in detecting skin cancer, especially malignant melanoma.
Symptoms
The typical mole is a brown spot. But moles come in different colors, shapes and sizes:
- Color and texture. Moles can be brown, tan, black, red, blue or pink. They can be smooth, wrinkled, flat or raised. They may have hair growing from them.
- Shape. Most moles are oval or round.
- Size. Moles are usually less than 1/4 inch (about 6 millimeters) in diameter — the size of a pencil eraser. Rarely, moles present at birth (congenital nevi) can be much bigger, covering wide areas of the face, torso or a limb.
Moles can develop anywhere on your body, including your scalp, armpits, under your nails, and between your fingers and toes. Most people have 10 to 40 moles. Many of these develop by age 50. Moles may change in appearance or fade away over time. Hormonal changes of adolescence and pregnancy may cause moles to become darker and larger.
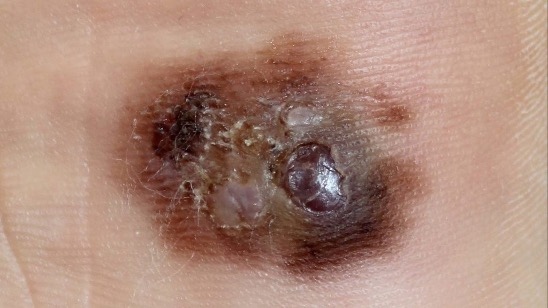
Unusual moles that may indicate melanoma
This ABCDE guide can help you determine if a mole or a spot may indicate melanoma or other skin cancers:
- A is for asymmetrical shape. One half is unlike the other half.
- B is for border. Look for moles with irregular, notched or scalloped borders.
- C is for color. Look for growths that have changed color, have many colors or have uneven color.
- D is for diameter. Look for new growth in a mole larger than 1/4 inch (about 6 millimeters).
- E is for evolving. Watch for moles that change in size, shape, color or height, especially if part or all of a mole turns black. Moles may also evolve to develop new signs and symptoms, such as itchiness or bleeding.
Cancerous (malignant) moles vary greatly in appearance. Some may show all of the features listed above. Others may have only one or two.
When to see a health care provider
Make an appointment with your health care provider if a mole looks unusual, grows or changes.
Causes
- Skin layers and melanin
Moles are caused when cells in the skin (melanocytes) grow in clusters or clumps. Melanocytes are distributed throughout your skin and produce melanin, the natural pigment that gives your skin its color.
Complications
Melanoma is the main complication of moles. Some people have a higher than average risk of their moles becoming cancerous and developing into melanoma. Factors that increase your risk of melanoma include:
- Being born with large moles. These types of moles are called congenital nevi. On an infant, such moles are classified as large if they're more than 2 inches (5 centimeters) in diameter. Even a large mole seldom becomes cancerous and almost never before the child reaches puberty.
- Having unusual moles. Moles that are bigger than a common mole and irregular in shape are known as atypical (dysplastic) nevi. They tend to be hereditary. And they often have dark brown centers and lighter, uneven borders.
- Having many moles. Having more than 50 ordinary moles indicates an increased risk of melanoma. Two studies add to the evidence that the number of your moles predict cancer risk. One showed that people under 50 years old who have 20 or more moles on their arms are at increased risk of melanoma. Another showed a relationship between the number of women's moles and breast cancer risk.
- Having a personal or family history of melanoma. If you've had melanoma before, you are at increased risk of a mole becoming cancerous. In addition, some types of atypical moles lead to a genetic form of melanoma.
Prevention
The following measures can help limit the development of moles and the main complication of moles — melanoma.
Watch for changes
Become familiar with the location and pattern of your moles. Regularly examine your skin to look for changes that may signal melanoma. Do self-exams once a month, especially if you have a family history of melanoma. With the help of mirrors, do a head-to-toe check, including your scalp, palms and fingernails, armpits, chest, legs, and your feet, including the soles and the spaces between the toes. Also check your genital area and between your buttocks.
Talk with your doctor about your risk factors for melanoma and whether you need a professional skin exam on a routine basis.
Protect your skin
Take measures to protect your skin from ultraviolet (UV) radiation, such as from the sun or tanning beds. UV radiation has been linked to increased melanoma risk. And children who haven't been protected from sun exposure tend to develop more moles.
- Avoid peak sun times. For many people in North America, the sun's rays are strongest between 10 a.m. and 4 p.m. Schedule outdoor activities for other times of the day, even on cloudy days or in winter.
- Use sunscreen year-round. Apply sunscreen about 30 minutes before going outdoors, even on cloudy days. Use a broad-spectrum sunscreen with an SPF of at least 15. Apply it generously and reapply every two hours — or more often if you're swimming or sweating. The American Academy of Dermatology recommends using a broad-spectrum, water-resistant sunscreen with an SPF of at least 30.
- Cover up. Sunglasses, broad-brimmed hats, long sleeves and other protective clothing can help you avoid damaging UV rays. You might also want to consider clothing that's made with fabric specially treated to block UV radiation.
- Avoid tanning lamps and beds. Tanning lamps and beds emit UV rays and can increase your risk of skin cancer.
This article is written by Mayo Clinic Staff. Find more health and medical information on mayoclinic.org.