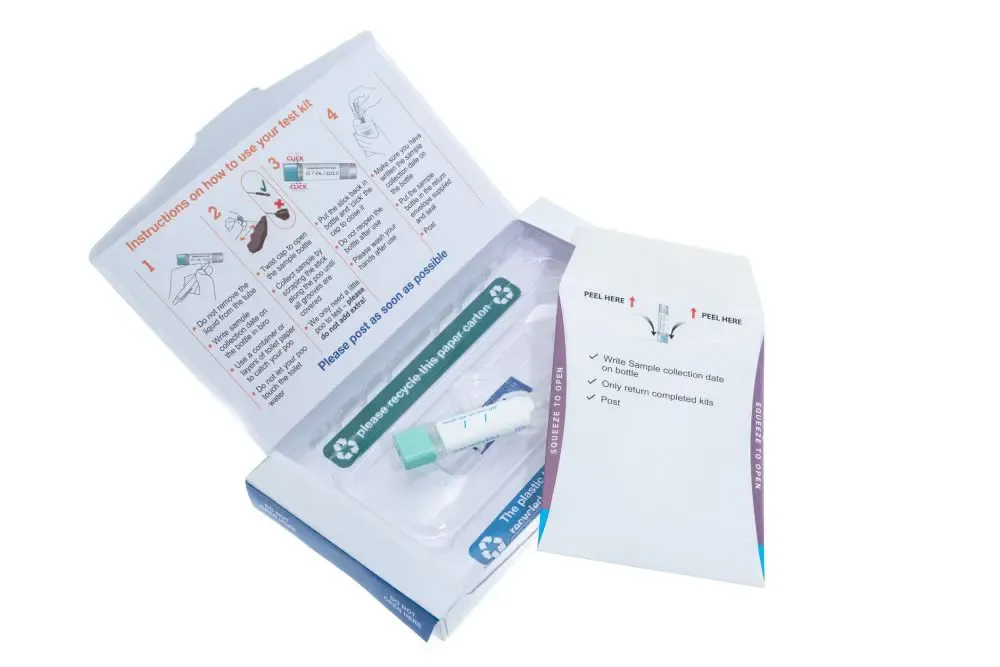
An at home colon cancer test (fecal occult blood test), also referred to as an FOBT, is a type of screening that checks for the presence of blood in a stool sample. Occult blood cannot be seen from a visual inspection. A stool sample must be submitted to a lab for further analysis. The FOBT screening checks for the microscopic presence of blood and can help doctors diagnose benign conditions, such as hemorrhoids or polyps. Screening may also detect cancer.
What Stool Tests Are Available, and How Do you Collect a Stool Sample?
- A guaiac FOBT (gFOBT) is used to identify the presence of heme (a component of hemoglobin) in a stool specimen. Using applicator sticks, samples from two to three different bowel movements are smeared onto a paper card coated with guaiac and returned to a doctor or lab for testing. During lab testing, hydrogen peroxide is added to the card. If blood is present, the test card will turn blue, which signifies a positive test result.
To avoid a false positive, your doctor may ask you to stop eating foods that contain heme in the days before testing. Heme can be found in red meat, poultry, and seafood. Vitamin C, iron supplements, turnips, and horseradish may also trigger false-positive results. Speak with your doctor for specific instructions on diet and medications, such as the use of nonsteroidal anti-inflammatory drugs (NSAIDs).
- Fecal immunochemical testing (FIT or iFOBT) is more widely used for colorectal cancer screening because of its cost and increased sensitivity. A fecal sample is scraped with a small probe. The collected matter is inserted into a sampling bottle or tube and returned to the lab. Testing uses antibodies that bind to hemoglobin protein, indicating whether blood is in the stool.
The FIT typically does not require any changes to diet. However, NSAIDs and other medications may affect test results. It is best to consult with your healthcare provider about what to avoid or modify before the test.
- A stool DNA test (FIT-DNA) combines the FIT with an additional search for altered DNA in the sample. DNA comes from the cells that line the colon and rectum, which are shed during a bowel movement. A laboratory can then extract DNA from the stool to identify the presence and scope of any mutated or abnormal genes.
Administering any of these tests during menstruation can produce a false positive.
All three of these screening tests are approved by the US Food and Drug Administration. The collection methods referenced above are typical but may vary according to test kit manufacturers. It’s essential to follow the directions and ensure kits are used before the expiration date.
The American Cancer Society recommends that adults of average risk for colorectal cancer start screening at age 45. If an individual is at increased risk due to inherited conditions or lifestyle choices, a doctor may recommend getting screened for colorectal cancer earlier. From ages 76 to 85, discuss with a doctor whether screening should continue. After age 85, screening is no longer recommended.
The gFOBT or FIT tests are recommended once a year. The FIT-DNA test is recommended once every three years.
What Do the Results Mean?
Blood in the stool is not a confirmation of cancer. Many conditions, including anemia, inflammatory bowel disease, ulcers, hemorrhoids, polyps, or anal fissures, may show gastrointestinal bleeding. Additional testing is typically required to determine the cause if a positive test result is found. A negative result indicates that no blood was found in the sample. An inconclusive result suggests that there may have been an issue with specimen collection, and your provider may request that you repeat the screening.
Because there is a risk factor for either a false-positive or false-negative result, always discuss your best options with a doctor. Despite the risk, the National Cancer Institute points to probable benefits, “Studies show that some screening tests for colorectal cancer help find cancer at an early stage and may decrease the number of deaths from the disease.”
Are Black Stools a Sign of Cancer?
Black, tarry bowel movements may be caused by diet changes or the introduction of a new medication. Some harmless reasons your stool may look darker include consumption of the following:
- Iron supplements
- Black licorice
- Dark chocolate
- Blueberries
- Dark food coloring additives
- Medications that include bismuth, such as Pepto Bismol® and Kaopectate®
The discoloration will stop once the food or medicine causing it is no longer used.
Other medical reasons for black stools include ulcers, esophageal tears or swollen veins, or cancer. Always consult your doctor for suspected or evident bleeding, even when you think you may know the reason.
What Other Colorectal Cancer Screening Tests Are Available?
Flexible sigmoidoscopy is a procedure that utilizes a small tube-like instrument with a light and lens to look inside the rectum and lower (sigmoid) colon for polyps or other abnormalities. Polyps or tissue samples may be removed and checked for signs of cancer. A sigmoidoscopy may sometimes be preferred over a colonoscopy because the test takes less time (about 15 – 20 minutes) and is less invasive. It generally does not require an anesthetic, though your physician may provide a relaxant. To prepare, you may need to maintain a liquid diet up to 24 hours before the test, and you will need to empty your colon either by enema or strong laxatives before the test. If your doctor finds polyps, they can be removed, but you will likely need a colonoscopy to examine the entire colon.
Colonoscopy also utilizes a thin tube with a lens. However, this test is more extensive and examines the entire colon. Your practitioner will remove polyps or other tissues for biopsy. An anesthesia specialist may also be present to provide conscious or deep sedation.
Your colon needs to be as clean as possible. Your health care provider will provide instructions which may include:
- Fasting from solid foods for 1 – 3 days
- An enema or strong laxatives to empty the colon. You can expect several bowel movements and should plan for rest, limited activity, and proximity to a bathroom during the cleanse.
This colonoscopy itself may take between 30 and 60 minutes.
Virtual colonoscopy, also known as computed tomography colonography or CTC, takes pictures of the colon through a series of x-rays or tomography. This screening also requires a complete cleansing. Digital images are assembled and analyzed for polyps or other irregularities. If polyps or other growths are found, a colonoscopy must be scheduled to remove them.
This screening may also capture possible issues with surrounding organs, such as kidneys, liver, spleen, and pancreas, that may result in further testing.
Minnesota Oncology recommends colorectal cancer screening for early detection and prevention beginning at age 45 or earlier if a family history.
“There is some risk of receiving a false positive or having a complication in some of the screenings. However, it is important to consider all your possible risk factors for colorectal cancer. Early detection and early treatment of cancer, if found, can yield improved outcomes,” said Robert Delaune, MD at Minnesota Oncology.
The doctors and staff at Minnesota Oncology are here to help. We have served the Twin Cities for over 25 years.
Our mission is to combine the strength of hope with the power of science, one patient at a time.
We strive to deliver patient-centered, comprehensive, and compassionate care in community cancer centers using best practice, state-of the-art therapies and research, in order to be the premier provider of care for patients with cancer and blood disorders in the region.
Our team specializes in:
- Medical Oncology
- Hematology
- Radiation Oncology
- Gynecological Oncology/ Surgery
- Thoracic Oncology/ Surgery
- Breast Surgery
Sources:
- https://www.cancer.gov/types/colorectal/patient/colorectal-screening-pdq#_13
- https://www.testing.com/tests/fecal-occult-blood-test/
- https://www.ncbi.nlm.nih.gov/books/NBK537138/
- https://www.sciencedirect.com/topics/nursing-and-health-professions/guaiac
- https://www.cancer.gov/types/colorectal/screening-fact-sheet#what-methods-are-used-to-screen-people-for-colorectal-cancer
- https://www.cdc.gov/cancer/colorectal/basic_info/screening/tests.htm
- https://www.webmd.com/digestive-disorders/black-tarry-stool-reasons
- Infographic: New Colorectal Cancer Screening Guideline for Men and Women at Average Risk
- https://www.cancer.net/navigating-cancer-care/diagnosing-cancer/tests-and-procedures/colonoscopy
- https://www.cancer.net/navigating-cancer-care/diagnosing-cancer/tests-and-procedures/sigmoidoscopy
- https://www.cancer.net/navigating-cancer-care/diagnosing-cancer/tests-and-procedures/fecal-occult-blood-tests